Understanding the skin barrier
The image that springs to mind when we read “skin barrier” may be cartoonish, with an impermeable layer of skin resisting entry of anything and everything. This is a false image projected by skin care companies trying to convince us that useful actives will not penetrate the skin unless we use sophisticated delivery systems, a gimmick to sell more products at higher prices. The truth of it is, whatever you apply to the skin will be absorbed, for better and for worse.
What is the skin barrier?
The term “skin barrier” refers to the main function of the skin: limiting water loss through the skin. How does the skin limit water loss? Live cells would not do the trick, so the cells in the interior of the epidermis will die, gradually, while experiencing major biochemical changes. The live cells of the stratum basale work with the chemicals they have available so that, by the end of the differentiation process (top of the figure), they don’t even look like cells anymore. The resulting layer is the stratum corneum.
The stratum corneum is a multilayered zone composed of flattened corneocytes that lack nuclei, surrounded by multiple planar lamellae sheets, enriched in waxy-type molecules like ceramides, cholesterol, and free fatty acids. This provides a lipid organization that makes the skin unique among biological membranes. So when we formulate a product to help protect the skin, we don’t need to imitate the chemistry of the skin. Skin ceramides, for example, are very complex lipids that you may not wish to imitate chemically in a skin care product. They are terribly expensive and have complex effects on the interior layers of the skin. What is required instead is the use of chemicals, natural or synthetic, with a waxy structure so that they will limit water loss like the skin’s ceramides.
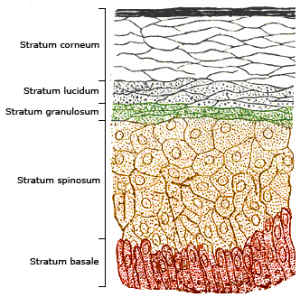
Figure. Skin cells change shape and structure to form the different layers of the skin. Cornified cells (corneocytes) are dead cells, but together they make a layer (horny layer, stratum corneum in Latin) that prevents water loss and the entry of microbes.
Not only does the stratum corneum limit water loss from the body, allowing us humans, organisms that depend totally on water, to walk around in an environment with very low humidity, but it also limits penetration of chemicals into the skin. Although this slows down absorption of nutrients (and noxious chemicals) applied topically, “limits penetration” does not mean that this layer is impermeable. This can be seen by observing water loss across the skin, which can be measured easily with laboratory instruments and increases with age and skin damage. In skin aged by sun exposure, absorption of external nutrients will be higher than in young skin, just like trans-epidermal water loss is higher. The skin is a barrier to losing water and to the entrance of microbes, but it is not impermeable.
Ingredient absorption through the skin barrier
How good is the skin as am actual barrier to the actives we need to apply to the skin? Not very good. After a shower, water soluble actives will enter the skin more readily. Actives will also enter through the pores and skin imperfections. Fat soluble actives will enter easily, especially when the carrier is suitable.
Even a low uptake of nutrients applied topically should substantially improve the health of skin deprived of such nutrients by the decrease of blood supply to the dermis that occurs in all of us as we age. You don’t need to absorb 100% of the useful actives applied topically. You don’t need delivery systems; your skin is permeable enough.
How far will these actives enter? They will get all the way to the external membrane of the live cells at the base of the skin. From there, the structure of the chemical will determine whether it can go further. Glucose, amino acids, and lipids will enter the cell because the cell needs them. Proteins can’t enter, but may still be able to exert an action on the cell if there is a receptor for the protein on the membrane. This is how epidermal growth factor (EGF) does its job. EGF will promote division of cells that have receptors for EGF by binding to the receptors at the cells’ surface and starting a cascade of biochemical events without anything actually penetrating. The culmination of this chemical cascade will be the activation of genes inside the nucleus.
Other chemicals that can’t enter the cell may do their job in the intercellular space, where enzymes are hard at work. Once they are within the intercellular space, enzymes transform these chemicals, hydrolyze esters, synthesize polyschharides, and do all kinds of chemical conversions. The products of these transformations will reach the live cells and enter them following the rules of permeability of that cell, as determined by the structure of the membrane.
A good reason to care about the skin barrier: atopic dermatitis
The terms eczema, atopic dermatitis or atopic eczema are used to describe a chronic inflammatory skin disease with allergic causes in which the skin itches and there is some scaling, crusting and/or oozing, rather than just erythema or inflammation. People who have eczema also tend to have other manifestations of allergy, like allergic rhinitis or asthma.
Atopic dermatitis affects about 10% of the US population and it can start as early as 2 months of age. Diseased skin is often characterized by a reduced barrier function and an altered lipid composition and organization. One possible reason why atopic dermatitis is such a widespread problem may be the emphasis our culture places on cleanliness. Soap and detergents will easily break the fragile skin barrier of a baby. And nothing good can be said about the crazy “treatments” that are out there, like microdermabrasion, microneedling, etc. Unless you have a very good reason not to, be very gentle with your skin.
The sensory interaction of the skin with the environment is also affected in these types of skin conditions, causing itching, stinging or even pain. The itchiness of eczema leads to scratching, and scratching leads to rashes. This vicious circle must be stopped because the scratching can lead to permanent changes in the skin, including scars, and infections.
We need our immune system to defend us from the infectious agents that are trying to invade us, like bacteria, viruses or fungi. However, skin affected by eczema is more prone to bacterial infection, as the skin barrier breaks down, facilitating attack by microorganisms. Atopy is characterized by high concentrations of serum immunoglobulin E (IgE), a high incidence of IgE-mediated responses on skin testing to common inhaled antigens, and many other manifestations of an oversensitive and “skewed” immune system.
For the time being, there is little that can be done about atopy at the molecular level, but if things get tough we can always go for one or more of the over-the-counter medicines available.
What can you do if you or a loved one has atopic dermatitis? It may help to avoid common allergens such as dust mites, animal danders and saliva, mold, and pollen. Immunotherapy, i.e. desensitization by “allergy shots”, does not seem to work for atopic dermatitis, in contrast to its relative success in treating patients with other allergic disorders.
Although cortisone is a good idea for emergencies, it cannot be used long-term because it may lead to skin thinning, depigmentation, and stretch marks. Also, topical corticosteroids may reach the blood stream, suppressing the activity of the adrenal glands.
Avoid factors that may worsen atopic dermatitis such as excessive bathing, low humidity environments, dry skin, rapid temperature changes, and exposure to solvents and detergents. After a bath or shower, apply an emollient product that will supplement the damaged skin barrier.
Lotions have a high water and low oil content and can worsen dry skin via evaporation, thus triggering flares of eczema. Conversely, thick, rich creams with a low water content, or ointments, which have zero water content, protect the skin better against dryness and eczema flares.
To alleviate the itching you can use calamine, or reach for Skin Actives Scientific’s Sea Kelp Coral, Rosehip or Pomegranate Seed Oil, or take a warm bath with Oat Beta Glucan and Rose Hip Oil. To decrease inflammation, use our Olive Ultra-Calming Cream. The fatty acids in Every Lipid Serum will provide essential nutrients for skin to repair the skin barrier.
-Dr. Hannah Sivak
